EKG Tutorial—From Atoms to Arrhythmias
Overview.
This approach is different from what you may have seen before, shaped by a clinical path rooted in bedside nursing and critical care rather than traditional classroom instruction.
It emerged from years of caring for unstable patients, making real-time decisions, and needing the EKG to be a reliable clinical tool—not an abstract pattern to memorize.
It was built from the bedside, not from a template.
That bedside-first mindset was forged in the mid-1970s, when our Program Director stepped into one of the country’s earliest Cardiac Intensive Care Units and had to learn—quickly—how to make the EKG mean something for the patient in front of him.
n 1975, when our Program Director went to work in one of the first Cardiac Intensive Care Units in the country, he found himself electrocardiographically underwater. Within a year, he was one of those in charge of the unit.
This course distills what he learned—and more importantly, how he learned to think about the integration of the heart and its electrocardiogram.
It took thirty years to research and three years to write. You’ll master it far more quickly—and with vastly more depth—than those who rely on pattern memorization alone.
You will learn:
A three-step method to confidently analyze any cardiac rhythm.
A three-step framework for 12-lead ECG interpretation.
The why behind every waveform, traced all the way down to the cellular and atomic level.
This foundation is what makes the knowledge durable. It lasts. And it empowers clinicians—regardless of prior experience—to perform at a high level quickly and confidently.
Along the way, electrophysiology is continuously tied to cardiac hemodynamics and diagnostic decision-making, deepening how you think about cardiology as a whole.


On-Site Tutorial Info→
Perform Like the Most Successful Professionals in Your Field
Who Will Benefit.
This tutorial adapts seamlessly to a wide clinical audience, including:
Cardiac Care & Critical Care Nurses
Emergency & Critical Care Clinicians
ACLS Paramedics
Cardiovascular & Advanced Practice Sonographers
EKG Technicians
Medical Students, Interns, and Residents
Researchers seeking physiologic clarity behind ECG findings.
Whether you want rapid mental protocols, a deeper physiologic explanation, or both—this experience meets you where you are.
Learning Objectives.
Upon completion, participants will be able to:
Explain what’s actually happening inside the cardiac cell—and why those unseen events create the EKG changes you see at the bedside.
Understand how electrolytes, membrane dynamics, and fluid shifts affect cardiac electrical activity and rhythm stability.
Connect each EKG waveform to a specific phase of cardiac contraction, not just its appearance on paper or screen.
Trace electrical flow through the heart and anticipate how conduction problems will show up clinically.
Place electrodes correctly and interpret each lead’s viewpoint, improving signal quality and diagnostic confidence.
Quickly determine axis and recognize chamber enlargement, especially when findings change from baseline.
Recognize bundle branch blocks and fascicular blocks and understand when they matter clinically.
Use a reliable, step-by-step method to analyze any rhythm, even under time pressure.
Identify all degrees of AV block and anticipate their clinical implications.
Distinguish ventricular tachycardia from SVT with aberrancy when the difference affects immediate management.
Recognize pre-excitation patterns and pacemaker behavior, normal and abnormal.
Identify medication, electrolyte, metabolic, and physiologic effects that commonly alter EKG appearance—and know when to escalate concern.
Topics Include:
Atomic and molecular structure as the foundation of all EKG activity.
Diffusion, osmosis, and active transport—and what the EKG actually records.
The cardiac cell membrane and its role in electrical and mechanical activity.
How—and why—the conduction system directs electrical flow.
Systematic diagnosis of arrhythmias with speed and certainty.
A confident, repeatable method for 12-lead EKG analysis.
Recognition, differentiation, and localization of ischemia and injury.
Conduction delays, blocks, and pre-excitation mechanisms.
Pacemaker function and EKG evaluation.
Electrolyte imbalance and pharmacologic EKG effects.
Athletic conditioning and hypothermia patterns.
Guided, in-class analysis of rhythm strips and 12-lead studies.
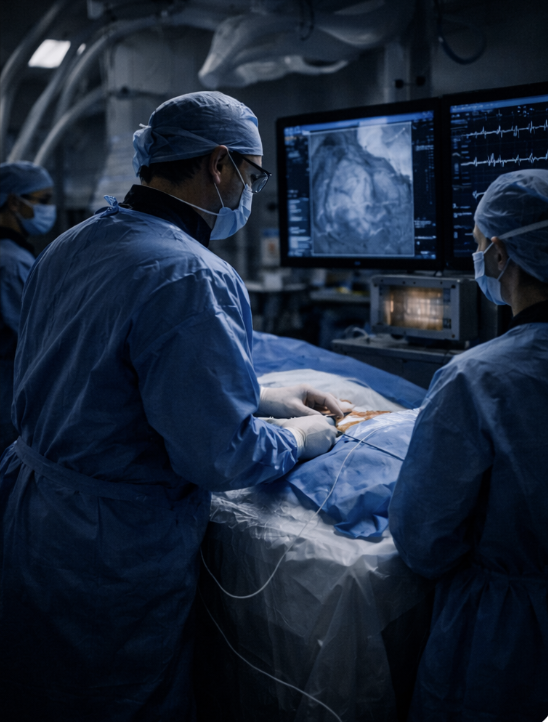
Clinical Impact by Care Setting.


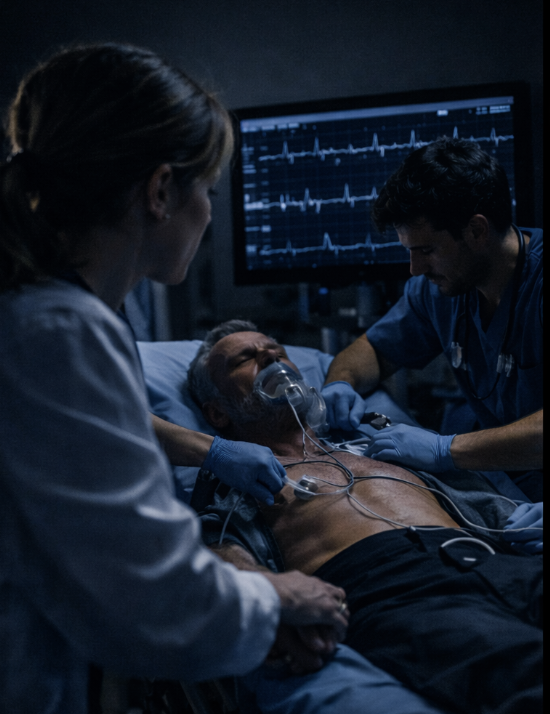




ICU nurses will better translate electrical signals into physiologic foresight.
ED nurses will better use the EKG as an early decision tool—not a retrospective report.
Telemetry nurses will better guard continuity and catch what others don’t see yet.
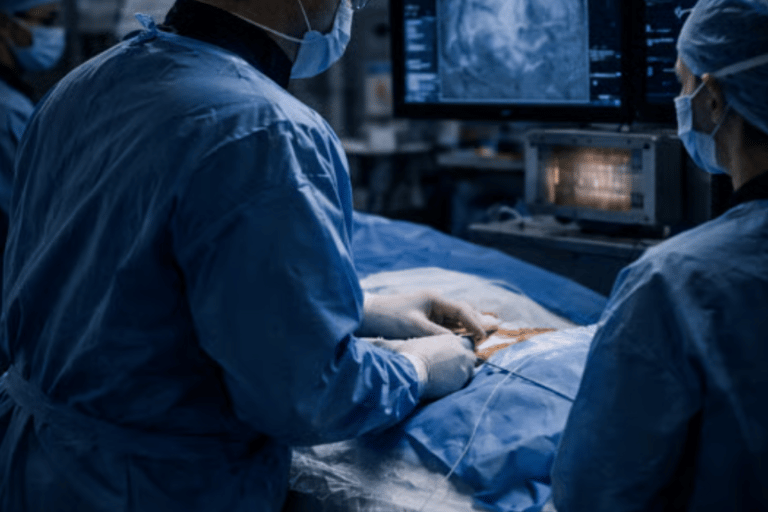
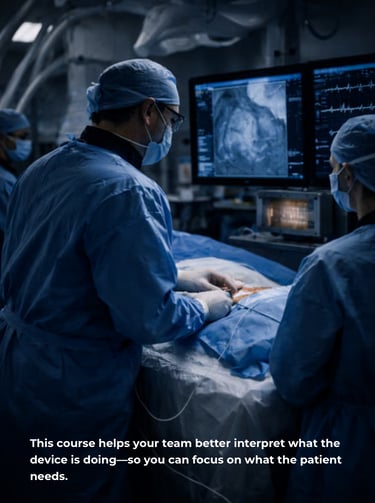
Your team will better interpret what the device is doing—so you can focus on what the patient needs.
On-Site Tutorial Info→
At 4 am you won't be all alone: you'll have elevated confidence to make, delay or defer the call for help.






Training Clinicians Worldwide Since 1981.
Testimonials reflect individual learning experiences. Growth in skill and confidence develops through guided training, continued practice, and personal commitment.
Contact
972 | 353-3200 USA Central Time
Course Campus:
4300 Wingren Drive
Irving (Las Colinas), Texas 75039
Mail | FedEx Address:
Box 101
Colleyville, TX 76034
Courses & Learning
Hands-On Clinical Courses
Ultrasound Physics
Cardiovascular Hemodynamics
EKG- From Atoms to Arrhythmias
Privacy Policy | Terms of Use. | Disclaimer
We’re committed to accessibility. View our Accessibility Statement.
The most powerful technology in medicine
is the person using it.
